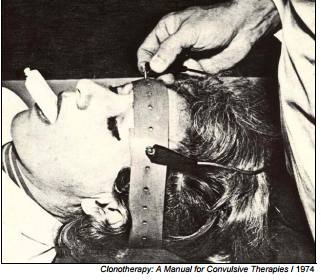
The Electroshock Quotationary®
Leonard Roy Frank, Editor
Publication date: June 2006
Copyright © 2006 by Leonard Roy Frank. All Rights Reserved.
Dedicated to everyone committed to
ending the use of electroshock
everywhere and forever
The Campaign for the Abolition of Electroshock in Texas (CAEST) was founded in
Austin during the summer of 2005. The Electroshock Quotationary (ECTQ) was created
to support the organization’s opposition to electroshock by informing the public,
through CAEST’s website, about the nature of electroshock, its history, why and how it’s
used, its effects on people, and the efforts to promote and stop its use. The editor plans
to regularly update ECTQ with suitable materials when he finds them or when they are
brought to his attention. In this regard he invites readers to submit original and/or
published materials for consideration (e-mail address: lfrank@igc.org).
CONTENTS
Acknowledgements
Introduction: The Essentials (7 pages)
Text: Chronologically Arranged Quotations (146 pages)
About the Editor
ACKNOWLEDGEMENTS
For their many kindnesses, contributions and suggestions to The Electroshock
Quotationary, I am most grateful to Linda Andre, Ronald Bassman, Margo Bouer, John
Breeding, Doug Cameron, Ted Chabasinski, Lee Coleman, Alan Davisson, Dorothy
Washburn Dundas, Sherry Everett, John Friedberg, Janet Gotkin, Ben Hansen, Wade
Hudson, Juli Lawrence, Peter Lehmann, Diann’a Loper, Rosalie Maggio, Jeffrey
Moussaieff Masson, Carla McKague, Jim Moore, Bob Morgan, David Oaks, Una Parker,
Marc Rufer, Sherri Schultz, Eileen Walkenstein, Ann Weinstock, Don Weitz, and Rich
Winkel.
INTRODUCTION: THE ESSENTIALS
I. THE CONTROVERSY
Electroshock (also known as shock therapy, electroconvulsive treatment, convulsive
therapy, ECT, EST, and ECS) is a psychiatric procedure involving the induction of a
grand mal seizure, or convulsion, by passing electricity through the brain. It is the most
controversial “treatment” in psychiatry, and perhaps in all of medicine.
Proponents call it a safe and highly effective way to address various kinds of “mental
illness” and certain medical conditions.
Opponents charge that it causes brain damage and is an instrument of social control,
sometimes administered by means of coercion or outright force and seldom with
genuine informed consent.
II. BACKGROUND
Since 1938, when Ugo Cerletti and Lucio Bini introduced the procedure at the University
of Rome, more than six million Americans and millions of others throughout the world
have undergone electroshock treatment.
Today, an estimated 100,000 people in the United States undergo ECT every year. Two-
thirds are women, and half are elderly. Age is not a disqualifying factor: there are
published reports of individuals as young as 34½ months and as old as 102 undergoing
the procedure (see in the text Bender’s entry in 1950 and the American Psychiatric
Association’s second entry in 1990).
A typical electroshock series for a hospitalized “patient” in the United States costs
between $50,000 and $75,000. An ECT series may also be administered on an
outpatient basis — in a hospital or in a psychiatrist’s office — at considerably less
expense: $1,500 to $2,000 per session. Government or private insurance usually covers
most, if not all, of the cost. Psychiatrists who specialize in electroshock often earn
$300,000 to $500,000 a year, considerably higher than the annual mean income for all
psychiatrists ($150,000).
The figures in the above two paragraphs suggest that in the United States alone
electroshock is a multi-billion-dollar-a-year industry.
To reduce the risk of relapse following an electroshock series, psychiatrists often urge
patients to pursue continuation (or maintenance) treatment. This generally involves
psychiatric drugs and often includes individual electroshocks as well, administered on
an outpatient basis at various intervals for six months or longer.
1
III. DIAGNOSES
The most common indication for electroshock is a diagnosis of clinical, or severe,
depression. An ECT series for depression typically consists of 6 to 12 sessions. People
diagnosed with schizophrenia or bipolar disorder (manic depression) may also be
subjected to electroshock, but this is less common; for such patients, a series of 15 to 25
sessions is standard. ECT is usually administered in the early morning, three times a
week (Mondays, Wednesdays, and Fridays).
Electroshock has also been administered to people with the following psychiatric
diagnoses: alcoholism, anorexia, anxiety disorder, catatonia, drug withdrawal
syndrome, homosexuality (no longer a psychiatric diagnosis), hysteria (ditto), narcotic
addiction, neurosis, obsessive-compulsive disorder, personality disorder, postpartum
depression, postpartum psychosis, psychosomatic disorder, pseudodementia, psychosis,
and substance abuse. In addition, ECT has been used to treat these medical conditions:
Alzheimer’s disease, backache, acute and chronic pain, delirium tremens, dementia,
epilepsy, mental retardation, neuroleptic malignant syndrome, Parkinson’s disease, and
psoriasis.
For persons said to be suicidal or in a state of depletion from lack of food (inanition),
electroshock is frequently the treatment of choice. For most psychiatric diagnoses,
however, it is the treatment of next resort (after one or more unsuccessful trials with a
psychiatric drug or combination of psychiatric drugs).
IV. METHOD OF ADMINISTRATION
Prior to the start of an electroshock series, the patient is given a psychiatric evaluation
and a physical examination. A consent form signed by the patient, a family member, or a
state-appointed guardian or conservator is almost always obtained after a psychiatrist
has explained to the designated signer the nature and effects of the procedure, the
manner of its administration, and why it has been deemed necessary. Some states
require a confirming opinion by a second physician. Some also require a judicial hearing
if the patient’s legal capacity to give or withhold consent is questionable, or if the patient
withholds consent.
A routine is followed for each session. The patient is asked to avoid food and drink for 8
to 12 hours beforehand. To prevent oral intake, each patient is usually kept under direct
staff observation. During this period, tranquilizers or sedatives may be used to reduce
the patient’s fear of and/or resistance to electroshock. Bladder and bowels are emptied
just before the session, and dentures, eyeglasses hairpins, earrings, and the like are
removed.
About 30 minutes beforehand, a conventional preanesthetic medication called atropine
is administered to dry secretions in the mouth and air passages, thus reducing the risk
of suffocation and other complications of swallowing one’s own saliva.
2
Shortly afterward, the patient is taken to the treatment room and put on a bed, padded
table, or gurney. Electrolyte jelly is applied to the two areas of the head, usually the
temporal areas, where the electrodes are to be placed. The jelly increases conductivity
and prevents burns. An intravenous line is started, and sensors are placed on the head
and chest to monitor brain and heart activity. A cuff is wrapped around the patient’s
upper arm to record blood pressure.
The patient is then anesthetized for 10 to 15 minutes with a short-acting barbiturate,
commonly Brevital (methohexital). Once the patient is unconscious, the muscle relaxant
Anectine (succinylcholine) is injected to reduce the risk of fractures, joint dislocations,
and damage to skeletal muscle, tendons, and ligaments, which were very common
before this modification became routine during the 1950s. Anectine causes an almost
complete paralysis of the body, including the respiratory system, so that the patient
must be supplied oxygen through a mask (oxygenation) until the Anectine wears off and
the patient is able to resume breathing on his or her own.
The anesthetic is not used to spare the patient pain because the shock itself, if strong
enough, produces instant unconsciousness and is therefore painless. Instead, the
anesthetic’s purpose is to eliminate the sensation of suffocation that the patient, without
an anesthetic, would experience as the muscle relaxant gradually took effect.
ECT without anesthetics and muscle relaxants is now referred to as unmodified or
classical ECT; the version with anesthetics, muscle relaxants (also called muscle
paralyzers), oxygenation, and monitoring is called modified ECT. Unmodified ECT is
now rare in the United States and Europe but is still common in developing countries
because of its lower cost.
Just before the convulsion, a rubber gag is inserted in the patient’s mouth to prevent
broken teeth and tongue-biting. Two electrodes wired to the shock machine are then
positioned on the head and may be held in place by an elastic headband.
The preparations having been completed, the psychiatrist presses a button on the shock
machine, releasing 70 to 500 volts (or more) of electricity for .02 second to 8 seconds.
The electric current penetrates the patient’s skull and passes through the brain, causing
a grand mal convulsion that lasts for 30 seconds to a minute and sometimes longer.
The patient then is taken to the recovery room in a comatose state, from which she or he
usually revives in 10 to 20 minutes. Ordinarily, the patient is able to leave the recovery
room 30 to 60 minutes later.
V. EFFECTS
Once conscious, the patient experiences one or more of the following adverse effects:
headache, dizziness, nausea, confusion, disorientation (not knowing who or where one
is or what time or day it is), muscle ache and soreness, physical weakness, memory loss,
euphoria, increased or irregular heartbeat (especially among the elderly), brief or
3
prolonged apnea (inability to breathe), and brief or prolonged cyanosis (blue skin from
loss of oxygen). Some of these effects may be so severe, even life-threatening, that
emergency treatment is necessary. For this reason, ECT is typically given in a hospital,
where such equipment is readily available.
After an electroshock session, patients may become “agitated,” or furious, when they
realize what has happened to them. Others become delirious or actively hostile,
prompting the use of mechanical and/or chemical restraints. Within a few hours, most
of the immediate adverse effects dissipate. Those that don’t may continue throughout
the day, for several days, or longer. During the recovery period, patients are often
prevented from or asked to refrain from driving, conducting legal or business
transactions, and engaging in other activities requiring alertness and memory.
It is the longer-term, and possibly severe and permanent, adverse effects of electroshock
that are most troublesome and frightening to patients and their families. The worst of
these, or at least the two that receive the most attention, are memory loss and learning
disability (inability to learn or retain new information). The former is called retrograde
amnesia; the latter, anterograde amnesia.
An ECT series causes a cumulative eradication of memory, which begins with recent
events, learning, beliefs, and thoughts, and gradually extends to the distant past. In time
some memories are recovered, usually within a month or two following the last ECT,
although the memories lost during the treatment period are most often permanently
erased. Most of the remaining gaps are filled only partially, if at all, through relearning.
Patients’ relearning involves talking with people they have known, reviewing documents
from their past (letters, diaries, school and work papers, home movies, newspapers,
books, and so on), and studying areas of interest with which they had once been
familiar. Reacquisition of lost skills may be achieved to some degree through study and
practice. The process of relearning is made more difficult because of the learning
disability caused by ECT.
Some patients do not seem to mind their ECT-induced memory problems; they may
even be largely, or completely, unaware of them. Others may welcome the loss of
memories because some were so troubling and disheartening. At the other extreme are
those for whom the memory loss is catastrophic, making their previous way of being,
lifestyle, and work no longer possible. In between are persons who adjust as best they
can to varying degrees of disability.
Physicians usually regard memory impairment, particularly when pronounced, as a sign
of brain damage (see in the text Sterling’s entry in 2001, and the cross-references
following his citation for more information about ECT-caused brain damage). Memory
loss may be accompanied by apathy, emotional dullness (blunted emotion, flat affect),
cardiovascular problems, spontaneous seizures, amenorrhea, demoralization,
dependency, and hopelessness; reduced ability to think, problem-solve, concentrate,
and connect with others; loss of personality; and loss of creativity, energy, enthusiasm,
moral awareness, and other elements that contribute to the individual’s sense of wellbeing
and worth. The patient’s age and physical condition, together with the intensity,
4
duration, number, and spacing of the individual convulsive procedures, determine the
severity and persistence of these effects.
Electroshock can also be fatal. Estimates of ECT-related death rates vary widely. The
lower estimates include:
•
1 in 10,000 (see in the text Boodman’s first entry in 1996)
•
1 in 1,000 (Impastato’s first entry in 1957)
•
1 in 200, among the elderly, over 60 (Impastato’s in 1957)
Higher estimates include:
•
1 in 102 (see in the text Martin’s entry in 1949)
•
1 in 95 (Boodman’s first entry in 1996)
•
1 in 92 (Freeman and Kendell’s entry in 1976)
•
1 in 89 (Sagebiel’s in 1961)
•
1 in 69 (Gralnick’s in 1946)
•
1 in 63, among a group undergoing intensive ECT (Perry’s in 1963-1979)
•
1 in 38 (Ehrenberg’s in 1955)
•
1 in 30 (Kurland’s in 1959)
•
1 in 9, among a group undergoing intensive ECT (Weil’s in 1949)
•
1 in 4, among the very elderly, over 80 (Kroessler and Fogel’s in 1974-1986)
The reasons for the difficulty in estimating ECT-related deaths include the following:
•
There is no central tracking of ECT-related deaths.
•
Some psychiatrists and hospitals underreport the number of ECT-related deaths.
•
Some psychiatrists and pathologists do not recognize deaths occurring during or
soon after ECT as ECT-related.
•
Families often refuse to authorize autopsies of relatives who have died during or
soon after ECT.
•
Professional journals are disinclined to publish reports or studies of ECT-related
deaths. Not since 1957 has any journal published a large-scale study of ECT-
related deaths (see in the text Impastato’s first entry in 1957).
•
It is difficult to determine with certainty, or near certainty, that ECT was the
cause of a patient’s death because multiple causes are often involved.
•
Deciding whether or not a patient’s death is ECT-related is difficult to establish
because there is no accepted time interval between a death and the last
electroshock he or she received. For example, is it an ECT-related death only if
the patient dies within a few minutes of undergoing ECT or may the interval be a
specific number of hours, days, or weeks up to a year?
VI. DOES ELECTROSHOCK WORK?
Opponents charge that ECT is demonstrably harmful and has not been proven effective
(even by psychiatric standards) for any more than a month or two. However, some
patients who have undergone electroshock, their families, and psychiatrists assert that
5
the procedure has been helpful. In evaluating their reports, opponents urge
consideration of the following:
•
Patients may feel better because of the well-known placebo effect. Any treatment
offered by a doctor, along with the suggestion that it will work, may have the
effect of making a patient feel better, at least for a while.
•
Patients may say they feel better (even when they don’t) for a variety of reasons:
because it’s expected of them, because they want to please their psychiatrists or
relatives, or because they fear that speaking truthfully would result in further
ECT or other sanctions.
•
Due to ECT-induced memory loss, patients may forget what had been bothering
them; as a consequence, they may feel less troubled and complain less to others.
•
Due to ECT-induced memory loss, patients may forget their ideas, beliefs, and
forms of conduct that others had found objectionable, including resistance to
being confined in a psychiatric facility and subjected to electroshock treatment.
This phenomenon may be called the brainwashing effect.
•
Family, friends, psychiatrists, and hospital staff may feel sympathy for ECT
patients and give them more consideration and better care.
•
Patients who believe the claims of psychiatrists and agree to undergo ECT may
give up so much self-respect, health, memory, intelligence, money, skills, or faith
that they refuse admit to themselves or others they are worse off after ECT.
•
ECT-induced brain damage may be so severe that patients are unaware of their
losses.
•
ECT-induced brain damage may result in a brief period of euphoria during
which the depression seems to lift, so for a time patients may indeed feel better.
•
ECT patients typically become dependent on others and more docile, more
cooperative, and easier to get along with as they recover from the treatment.
•
Because ECT deadens the emotions, patients whose everyday lives are filled with
tension, anger, sadness, and misery may experience temporary relief.
VII. WELL-KNOWN ELECTROSHOCK PATIENTS
Some of the better-known people who have undergone electroshock treatment include
French philosopher Louis Althusser, French playwright and actor Antonin Artaud, actor
Clara Bow, writer and poet Richard Brautigan, television personality Dick Cavett, Kitty
Dukakis (Massachusetts governor Michael Dukakis’s wife), Missouri senator and
(briefly) 1972 Democratic Party vice presidential nominee Thomas Eagleton, writer
Ralph Ellison, actor Frances Farmer, New Zealand writer Janet Frame, singer Connie
Francis, singer and actor Judy Garland, Naomi Ginsberg (Allen Ginsberg’s mother),
Australian pianist David Helfgott, writer Ernest Hemingway, Russian-born U.S. pianist
Vladimir Horowitz, Irish poet Pat Ingoldsby, poet Bob Kaufman, musician Roland
Kohloff, Olga Koklova (Pablo Picasso’s first wife), writer Seymour Krim, British actor
Vivien Leigh, pianist and actor Oscar Levant, poet Robert Lowell, British humorist Spike
Milligan, composer Paul Moravec, physician and writer Sherwin Nuland, actor Jennifer
O’Neill, English writer and illustrator Mervyn Peake, baseball player Jimmy Pearsall,
writer Robert Pirsig, poet Sylvia Plath, composer Cole Porter, poet and lyricist Dory
6
Previn, songwriter and performer Lou Reed, singer/actor and human rights leader Paul
Robeson, French fashion designer Yves Saint-Laurent, writer Andrew Solomon, writer
William Styron, actor Gene Tierney, songwriter and performer Townes Van Zandt,
physician Mark Vonnegut (Kurt Vonnegut’s son), poet John Wieners, Rose Williams
(Tennessee Williams’s sister), British writer Simon Winchester, CIA official Frank
Wisner, Australian singer Stevie Wright, and singer Tammy Wynette.
VIII. OVERVIEW
While media reports suggest that electroshock use in the United States is increasing,
there is a growing grassroots movement demanding that the procedure be abandoned or
abolished.
